**Malaria Overview:**
– Signs and symptoms include fever, fatigue, vomiting, and headaches.
– Severe cases may lead to jaundice, seizures, coma, or death.
– Recurrences of the disease can happen if not properly treated.
– Milder symptoms occur upon reinfection after surviving an infection.
– Malaria is caused by parasites in the genus Plasmodium, with P. falciparum and P. vivax being common.
– Different species of Plasmodium can cause varying severity of malaria.
**Complications and Diagnosis:**
– Complications of malaria include respiratory distress, kidney failure, cerebral malaria, enlarged organs, and low blood sugar.
– Diagnosis methods include microscopic examination of blood, rapid diagnostic tests, and polymerase chain reaction tests.
– Prevention methods involve mosquito nets, insect repellents, and various medications.
– Concerns include drug resistance in some regions.
**Global Impact and Recurrent Malaria:**
– In 2022, there were 249 million malaria cases worldwide, with 608,000 deaths, mostly in Sub-Saharan Africa.
– Children under five are at high risk, with preventable deaths occurring every minute in 2021.
– Recurrent malaria includes recrudescence, relapse, and reinfection.
– Immunity may develop with frequent exposure to malaria.
**Pathophysiology and Genetic Resistance:**
– Malaria infection involves liver and red blood cells phases.
– Genetic factors like sickle cell trait and thalassaemia provide resistance to malaria.
– Human genetic resistance to malaria has evolved due to high mortality.
**Prevention and Control Strategies:**
– Prevention methods include medication, mosquito control, and bite prevention.
– Vector control methods like insecticide-treated nets, indoor residual spraying, and house modifications are effective.
– Mass drug administration and research on malaria vaccines are ongoing strategies.
– Community strategies like health education and early disease recognition are crucial in malaria control.
Malaria is a mosquito-borne infectious disease that affects humans and other vertebrates. Human malaria causes symptoms that typically include fever, fatigue, vomiting, and headaches. In severe cases, it can cause jaundice, seizures, coma, or death. Symptoms usually begin 10 to 15 days after being bitten by an infected Anopheles mosquito. If not properly treated, people may have recurrences of the disease months later. In those who have recently survived an infection, reinfection usually causes milder symptoms. This partial resistance disappears over months to years if the person has no continuing exposure to malaria.
| Malaria | |
|---|---|
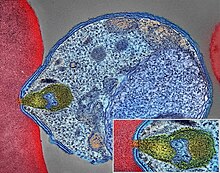 | |
| Malaria parasite connecting to a red blood cell | |
| Pronunciation | |
| Specialty | Infectious disease |
| Symptoms | Fever, vomiting, headache, yellow skin |
| Complications | seizures, coma, organ failure, anemia, cerebral malaria |
| Usual onset | 10–15 days post exposure |
| Causes | Plasmodium transmitted to humans by Anopheles mosquitoes |
| Diagnostic method | Examination of the blood, antigen detection tests |
| Prevention | Mosquito nets, insect repellent, mosquito control, medications |
| Medication | Antimalarial medication |
| Frequency | 247 million (2021) |
| Deaths | 619,000 (2021) |
Human malaria is caused by single-celled microorganisms of the Plasmodium group. It is spread exclusively through bites of infected female Anopheles mosquitoes. The mosquito bite introduces the parasites from the mosquito's saliva into a person's blood. The parasites travel to the liver where they mature and reproduce. Five species of Plasmodium commonly infect humans. The three species associated with more severe cases are P. falciparum (which is responsible for the vast majority of malaria deaths), P. vivax, and P. knowlesi (a simian malaria that spills over into thousands of people a year). P. ovale and P. malariae generally cause a milder form of malaria. Malaria is typically diagnosed by the microscopic examination of blood using blood films, or with antigen-based rapid diagnostic tests. Methods that use the polymerase chain reaction to detect the parasite's DNA have been developed, but they are not widely used in areas where malaria is common, due to their cost and complexity.
The risk of disease can be reduced by preventing mosquito bites through the use of mosquito nets and insect repellents or with mosquito-control measures such as spraying insecticides and draining standing water. Several medications are available to prevent malaria for travellers in areas where the disease is common. Occasional doses of the combination medication sulfadoxine/pyrimethamine are recommended in infants and after the first trimester of pregnancy in areas with high rates of malaria. As of 2023, two malaria vaccines have been endorsed by the World Health Organization. The recommended treatment for malaria is a combination of antimalarial medications that includes artemisinin. The second medication may be either mefloquine, lumefantrine, or sulfadoxine/pyrimethamine. Quinine, along with doxycycline, may be used if artemisinin is not available. In areas where the disease is common, malaria should be confirmed if possible before treatment is started due to concerns of increasing drug resistance. Resistance among the parasites has developed to several antimalarial medications; for example, chloroquine-resistant P. falciparum has spread to most malarial areas, and resistance to artemisinin has become a problem in some parts of Southeast Asia.
The disease is widespread in the tropical and subtropical regions that exist in a broad band around the equator. This includes much of sub-Saharan Africa, Asia, and Latin America. In 2022, some 249 million cases of malaria worldwide resulted in an estimated 608000 deaths, with 80 percent being five years old or less. Around 95% of the cases and deaths occurred in sub-Saharan Africa. Rates of disease decreased from 2010 to 2014, but increased from 2015 to 2021. According to UNICEF, nearly every minute, a child under five died of malaria in 2021, and "many of these deaths are preventable and treatable". Malaria is commonly associated with poverty and has a significant negative effect on economic development. In Africa, it is estimated to result in losses of US$12 billion a year due to increased healthcare costs, lost ability to work, and adverse effects on tourism.
